Regulation and Employer Benefits Plans
How ERISA and a complex web of state insurance laws have created the modern employer health benefits program
Note: We’re going to focus on employer-provided insurance, but I’m not a health insurance broker, nor am I a lawyer, so this should not be constituted as advice in any way. Instead, these are just fun words on a page, for entertainment purposes.
I’m going to let you in on a secret of the insurance industry. Most people believe that their health coverage is provided by a health insurance carrier. But if you’ve worked at a large company, odds are that your insurer was actually your company. These days, most employer-provided health insurance stems from self-insured companies rather than major insurance carriers, and insurance companies have transformed themselves to focus not only on taking on risk, but also to provide services and products for other risk-bearing entities.1 In this article, we’re going to explore why that’s happened.
First, we need to talk about how health insurance as a packaged product works. In the wild, insurance is a huge and complicated machine with a variety of vendors, consultants, and contractors, but at the end of the day, it boils down to two functions that insurance companies perform.
1) Pool and take on the risk for the company’s employees.
2) Perform (or contract) all of the administrative work, including, but not limited to the following responsibilities:
Provider network-building and negotiation
Claims management
Drug management (through PBMs)
Utilization management (prior authorization, claims audits, step therapy)
Care navigation (or… they at least try)
Distribution of health plan IDs
Regulatory paperwork, licensing, and insurance taxes
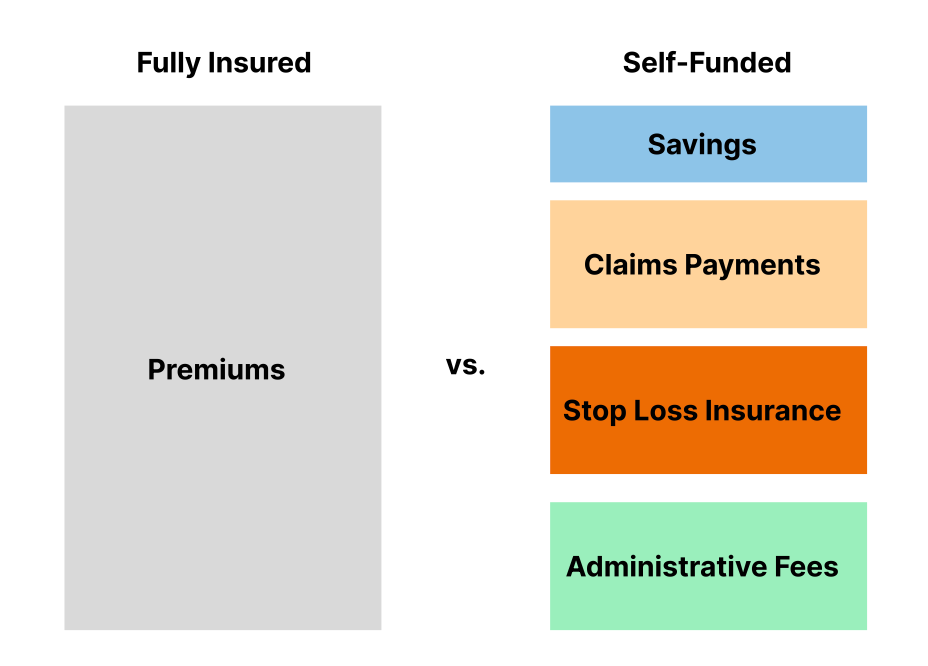
When a fully-insured insurance product is purchased, an employer will pay a single, fixed-price premium for all of these services. But when an employer unbundles the set of products, and purchases them separately, or even purchases them together but acts as the risk-bearing agent instead of an insurance carrier, their costs go down and they almost always save money.
Source: me and my mad Figma skills
Employers have taken notice of the additional savings, and, over the past 20 years, almost all large employers have switched from purchasing fully-insured products to self-insuring their health plans. These savings stem partially from the additional complexity and work that the employer is taking on, but there’s something far more interesting going on, and that has to do with the regulatory nature of insurance. To really understand where these savings come from, we need to dive into a law called ERISA.
In 1974, congress passed the Employee Retirement Income Security Act (ERISA). The main purpose of the legislation was to prevent employee pension funds from being run irresponsibly, in response to a slew of pension bankruptcies stemming from bad financial decisions by pension administrators. They focused on creating fiduciary responsibilities for these administrators, and set standards on what responsible stewardship requires. Since employer benefits plans were becoming increasing popular around the same time, and also required financial contributions from employers, legislators extended some of the fiduciary concepts over into employer benefits plans too.
ERISA established that employer benefits programs, defined as “any plan, fund, or program established or maintained by an employer to provide employees and beneficiaries” with health-related benefits, could not be regulated as insurance providers. On the other hand, ERISA did not provide a comprehensive regulatory framework for employer-funded health benefits plans. This created an unusual carveout with fairly permissive federal laws, but very limited ability to regulate at the state level due to federal preemption of state law.
As a quick aside, it may be interesting to review some of the ways in which ERISA does actively regulate employer benefits programs.2
Title I, Part 1: Plan sponsors and administrators must file an annual report with the Department of Labor, called a 5500 Series report, describing financial and operational activities of the plan, and they must provide beneficiaries and participants with an annual summary report of this filing.
Title I, Part 4: Plans must meet minimum standards for fiduciary conduct, such that persons who exercise discretionary authority or control over the management of a plan or its assets must act “solely in the interest of the plan participants and beneficiaries and for the exclusive purpose of providing benefits and defraying reasonable expenses of administering the plan.”
Title I, Part 5: Contains administration and enforcement provisions, including remedies available to plan beneficiaries and participants, and to the Department of Labor, for violations. It also describes the requirement for each plan to document procedures for the filing of benefit claims and appeal of denied claims.
Title I, Part 6: Continuation of coverage provisions as enacted in COBRA 1985, so that participants or beneficiaries who have had qualifying life events that cause loss of coverage, are able to continue receiving benefits for a certain amount of time.
Title I, Part 7: This part contains the provisions that regulate required benefits and treatment of plan participants, including HIPAA, which, beyond the data protection aspects, prevents discrimination against individuals with preexisting conditions or plan eligibility discrimination based on a health factor. It also contains the Newborns’ Act, which requires that plans offer benefits for mothers and children to stay overnight in the hospital after childbirth, the Mental Health Parity Act, which provides parity in dollar limits to mental health, and, amongst other regulations, GINA, or the Genetic Information Nondiscrimination Act.
Getting back to the conflict between state and federal rules, state legislators had a trick up their sleeves, thanks in part to the McCarran-Ferguson Act of 1945. This federal law delegated regulation of insurance to the state level. These regulators realized that instead of attempting to pass laws affecting the employer benefits plans themselves, they could regulate licensed insurers and the products they sold to employer benefits plans. This allowed states to create rules that would affect employers without touching them directly.
For example, states could not pass a law that required that employer benefits plans include fertility benefits, but they could require that all insurance products in the state do.3 By regulating insurance directly, states held carriers companies to a higher standard, requiring capital reserves requirements, premiums taxes, and consumer protection measures. This made insurance more expensive, and carriers passed these costs on to the employers.
However, this trick only works when the employer actually purchases an insurance product. If the employer acts as its own risk pool, and pieces together the functions of health insurance from non-risk-bearing vendors known as third party administrators (TPAs), they are exempt from state insurance laws. This means that self-funded insurance not only cuts out the middle man, but it reduces the set of applicable taxes and regulations from the state, making self-funded insurance generally cheaper than a comparable fully-insured product.
As a result, employers have shifted from purchasing full insurance products from licensed, regulated carriers, to piecing together their own coverage to save on taxes (government and vertical-integration margins) and have more control of their benefits packages. As we can see below in the graphics below, self-funded plans have become increasingly popular over time, especially with medium and large-sized employers.
Source: KFF Employer Health Benefits Survey, 20214
Source: KFF Employer Health Benefits Survey, 20215
Things can get a little complicated here, since the definition of self-insured can vary. Most insurance companies have reinsurance they purchase in case claims substantially exceed projections. Self-funded employers often use a similar mechanism, called stop-loss insurance, to keep outsized losses in check. If stop-loss insurance is set at a very low attachment point, where insurance is provided if claims exceed projections at all, then the employer isn’t actually taking on the risk of being an insurer- they’re contracting it out to another provider who is acting more as an first insurer than a reinsurer. As a result, many states have set rules around minimum attachment points for stop-loss insurance, but these regulations vary from state to state.6
NAIC created template legislature for multiple states, whereby a stop loss policy cannot be issued unless its aggregate attachment point for small groups is at least 120% of expected claims, and its specific attachment point is at least $20k.
North Carolina regulates stop-loss insurance the same way as regular insurance, enforcing licensing and rules for the industry.
New York and Delaware do not allow stop-loss insurance for small groups, requiring these employers to have more capital on hand in case claims exceed projections.
This variance in the regulatory environment creates a substantial advantage for large employers (and their diversified risk pools) as compared to small employers in moving from fully-insured to self-funded plans. Larger employers tend to be able to take on more complexity and more risk, so we see a variety of different patterns emerge depending on the capabilities and needs of the employer. Despite the complicated set of build-or-buy decisions and a large ecosystem catering to this market, employer benefits plans tend to fall into one of the following categories (I’m excluding PEOs and similar constructs for another time).
Fully-Insured Plan: Employers pay a fixed premium to a carrier each month in exchange for a fully packaged insurance product for the company’s employees.
Level-Funded Plan: Employers pay a fixed premium to a carrier each month, with part going to administrative fees, part to stop loss insurance, and part to pay claims. After a year, if the total amount of claims paid out by the carrier is less than the amount paid in by the employer, they will receive a rebate for the excess amount. Level-funded plans were the real mystery for me that got me interested in going down this path, because I couldn’t figure out how they provided cheaper premiums if they provided a fully-packaged product with stop-loss insurance. As it turns out, these plans are generally considered self-funded plans, and as a result, are not regulated or excise taxed at the state level.
ASO Plan: Employers work with existing insurance carriers and their networks for these administrative services only plans, but employers take on risk and only pay for claims when they come in. Large employers often use ASO plans, causing employees to believe that they “have insurance” from a major carrier, even though the carrier is simply allowing the employer to rent their network of providers and processing claims on the behalf of the employer.
Captive Programs: Groups of employers with comparable employee pools band together to mitigate risk from any one set of employees. These programs typically have a variety of consultants, brokers, and can work with carriers or TPAs to fulfill all of the needs for an insurance program. These captive programs work with TPAs or carriers to select networks and rates that are tailored for the needs of the overall employee base across all companies in the captive. These programs are also called Multiple Employer Welfare Arrangement (MEWA), and are more heavily regulated than traditional Single Employer or Union benefits plans, due to the strong possibility and history of fraudulent behavior attempting to get around state rules and regulations through ERISA preemption.
Fully Self-Insured: Employers work directly with benefits consultants and TPAs to select networks and rates that are tailored for their employee base. They pay claims directly out of pocket from a pre-allocated pool of money, but work with a stop loss insurer to prevent outsized losses. Typically, self-insured companies are able to retrieve their own claims data, which they then use to optimize their network, pricing, and overall spend, in conjunction with an army of benefits consultants and brokers. With great flexibility comes great power in cost reduction at scale, since these employers can negotiate for better rates in the services that their employee base really need. For example, employee bases that perform physical labor will want to negotiate for better rates with musculoskeletal providers like orthopedic surgeons and physical therapists, whereas stressed out consultants may be better served by more mental health benefits and coverage.
These options and configurations are serviced by a vast ecosystem of insurance carriers, TPAs, stop-loss insurers, clearinghouses, claims adjusters, brokers, and consultants-- some tech-enabled, and others more incumbent. As a result, it’s become easier to become self-insured than ever before.
This does have its downsides, though. Employer-provided insurance as a construct is uniquely American, stemming from taxation and wage caps during WWII. It’s created a system where Americans don’t internalize the cost of their own health care, but they are afraid of leaving jobs and losing their benefits. In my own experience, I’ve had great health insurance through all of my employers, but leaving to focus on learning healthcare, the quality of my insurance has dropped dramatically, and I’m still paying thousands of post-tax dollars a year for it. Because of the high degree of regulation on the individual and small group markets (despite government subsidies), the cost efficiency of my insurance is much lower than the cost efficiency of large group, self-employed markets. As a result, I’d love to see a regulatory overhaul addressing the parity issues between these markets, and a further federalization of insurance regulations to reduce the complexity of operating insurance across state lines.
We’ll dive deeper into the payer ecosystem in future articles. Thanks for reading along with me, and please let me know if you have any feedback or follow-up questions!
Patrick
Thanks to Russell Pekala and Jan-Felix Schneider for proof-reading and providing feedback!
For more details on ASO products and how carriers think about the different lines of revenue, I would recommend checking out the UHC 10K report from 2021: https://www.unitedhealthgroup.com/content/dam/UHG/PDF/investors/2021/UNH-Q4-2021-Form-10-K.pdf
https://www.dol.gov/sites/dolgov/files/ebsa/about-ebsa/our-activities/resource-center/publications/mewa-under-erisa-a-guide-to-federal-and-state-regulation.pdf
https://www.commonwealthfund.org/publications/issue-briefs/2022/may/state-cost-control-reforms-erisa-preemption
https://www.kff.org/report-section/ehbs-2021-section-10-plan-funding/
https://www.kff.org/report-section/ehbs-2021-section-10-plan-funding/
https://www.cga.ct.gov/2019/rpt/pdf/2019-R-0193.pdf